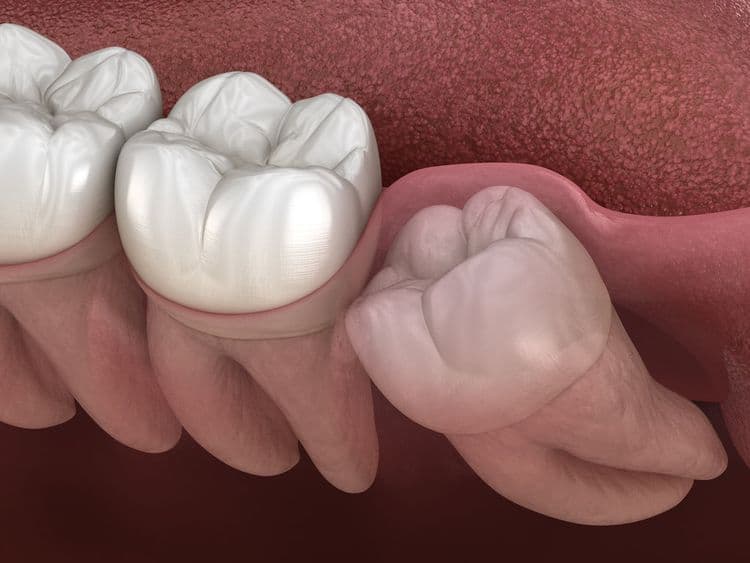
The potential link between wisdom teeth and high blood pressure is a subject of ongoing investigation. Emerging evidence suggests that impacted wisdom teeth may contribute to systemic inflammation due to associated periodontal disease, which is known to influence cardiovascular health. As periodontal pathogens circulate in the bloodstream, they might provoke inflammatory responses that impact vascular function. Despite the lack of definitive evidence, this intriguing connection warrants further exploration to understand its implications for patient care.
Understanding Wisdom Teeth and Their Role in Oral Health
Wisdom teeth, also known as third molars, are the last set of molars to erupt in the human dentition, typically emerging between the ages of 17 and 25. From a clinical perspective, their role in oral health remains debated, as they are often considered vestigial structures. In certain populations, wisdom teeth can contribute to efficient mastication; however, their location and potential impaction can complicate oral hygiene maintenance. The accumulation of plaque and bacteria around partially erupted or misaligned third molars increases the risk of periodontal disease and dental caries. Evidence suggests that meticulous oral hygiene practices, including regular brushing and interdental cleaning, are vital in mitigating these risks. Consequently, monitoring and managing wisdom teeth are essential components of thorough dental care.
The Common Problems Associated With Wisdom Teeth
As individuals reach late adolescence and early adulthood, the emergence of third molars often presents a variety of clinical challenges, necessitating careful evaluation by dental professionals. Impacted teeth, a common issue with wisdom teeth, occur when these molars fail to erupt properly due to spatial constraints or malalignment. This condition can lead to pericoronitis, characterized by inflammation and infection of the surrounding soft tissue. Additionally, impacted wisdom teeth are frequently associated with the formation of dental cysts, specifically dentigerous cysts, which can cause resorption of adjacent tooth roots and weaken the jaw structure. Early detection through radiographic imaging and clinical assessment is critical to managing these complications effectively. Such evaluations assist in preventing further oral health deterioration and guide appropriate intervention strategies.
Exploring the Link Between Oral Health and Systemic Conditions
Increasing evidence underscores a significant correlation between oral health and systemic conditions, highlighting the necessity for interdisciplinary collaboration among healthcare providers. Poor oral hygiene practices can exacerbate systemic inflammation, contributing to cardiovascular diseases, including hypertension. The presence of impacted wisdom teeth can lead to localized infections and inflammation, necessitating wisdom tooth extraction as a preventive measure. Evidence suggests that periodontal pathogens may enter the bloodstream, triggering systemic responses that potentially elevate blood pressure. Hence, maintaining ideal oral hygiene practices is paramount not only for oral health but also for systemic well-being. Healthcare professionals should consider thorough oral examinations as part of routine evaluations to mitigate risks associated with both dental and systemic health, fostering a holistic approach to patient care.
What Current Research Says About Wisdom Teeth and Blood Pressure
Current research indicates a correlation between oral health and systemic conditions, including hypertension. Studies have shown that dental inflammation, commonly associated with impacted or infected wisdom teeth, may contribute to elevated blood pressure by promoting systemic inflammatory responses. This evidence suggests the importance of addressing oral health issues in the management of cardiovascular risk factors.
Links Between Oral Health
Emerging research is shedding light on the potential connections between oral health and systemic conditions, specifically the role of wisdom teeth in influencing blood pressure. Studies indicate that compromised oral hygiene and inadequate dental care may exacerbate systemic health issues, including hypertension. Wisdom teeth, particularly when impacted or partially erupted, can complicate oral hygiene practices, potentially leading to periodontal disease. This condition may contribute to systemic inflammation, a factor implicated in elevated blood pressure. Clinical observations and epidemiological data suggest that maintaining ideal oral health could mitigate such risks. While the exact mechanisms remain under investigation, the interrelationship between dental health and systemic conditions underscores the importance of thorough dental care in overall health management. Further research is warranted to elucidate these complex interactions.
Impact of Dental Inflammation
Although often overlooked, dental inflammation associated with wisdom teeth presents a significant concern in the study of systemic health, particularly in its potential impact on blood pressure. Emerging evidence suggests a correlation between chronic dental inflammation, such as that caused by dental abscesses and periodontal disease, and elevated blood pressure levels. These conditions can instigate a systemic inflammatory response, releasing pro-inflammatory cytokines that contribute to vascular endothelial dysfunction. Studies have demonstrated that untreated periodontal disease is associated with increased risks of cardiovascular complications, including hypertension. The pathophysiological mechanisms underlying this association include bacterial translocation into the bloodstream, promoting systemic inflammation. Therefore, the presence of impacted or infected wisdom teeth may exacerbate inflammatory pathways, potentially leading to hypertension. Further longitudinal studies are warranted to elucidate these associations.
The Impact of Wisdom Teeth on Stress and Anxiety Levels
Frequently overlooked in discussions of dental health, wisdom teeth can exert a significant influence on an individual’s stress and anxiety levels. The eruption of wisdom teeth is often associated with discomfort and pain, leading to heightened stress responses. This physiological stress can contribute to elevated anxiety levels, necessitating effective anxiety management strategies. Clinical studies have shown that the anticipation of wisdom teeth extraction can exacerbate anxiety symptoms in patients. Additionally, complications such as impaction or misalignment of these teeth can further amplify psychological distress. Effective anxiety management during dental consultations is essential to mitigating these effects. As a result, dental practitioners should be aware of the potential psychosocial implications associated with wisdom teeth and incorporate stress reduction techniques to enhance patient care and overall well-being.
How Inflammation From Wisdom Teeth Can Affect Blood Pressure
The psychological stress associated with wisdom teeth is not the only concern; inflammation resulting from these teeth can also have physiological repercussions, particularly affecting blood pressure. When wisdom teeth become impacted or infected, they trigger an immune response characterized by inflammation. This inflammation can lead to the release of pro-inflammatory cytokines, which have been implicated in vascular changes that may elevate blood pressure. The systemic inflammation effects extend beyond localized discomfort, potentially exacerbating hypertension through vasoconstriction and increased arterial stiffness. Clinical studies have noted that the presence of chronic oral inflammation may correlate with elevated systolic and diastolic pressures. Therefore, the inflammation effects from wisdom teeth should be considered a contributory factor in the complex etiology of hypertension.

Expert Opinions on the Connection Between Wisdom Teeth and Hypertension
Clinical experts have identified a potential correlation between the persistent inflammation associated with impacted wisdom teeth and elevated blood pressure, suggesting that chronic oral inflammation may contribute to systemic vascular responses. Moreover, stress induced by oral discomfort can exacerbate hypertension, underscoring the significance of oral health management in patients with elevated cardiovascular risk. Evidence-based studies are ongoing to further elucidate these complex interactions and provide thorough guidelines for clinicians.
Inflammation and Blood Pressure
While the relationship between oral health and systemic conditions is well-documented, the potential link between wisdom teeth inflammation and hypertension warrants further investigation. Inflammation effects ensuing from impacted or infected wisdom teeth can potentially exacerbate systemic inflammatory responses. This localized inflammation may contribute to the release of pro-inflammatory cytokines, which have been implicated in vascular changes influencing blood pressure regulation. Clinical studies have noted correlations between chronic oral inflammation and elevated blood pressure, though causality remains to be definitively proven. Understanding the pathological mechanisms underlying these associations is essential for elucidating the role of oral inflammation in systemic hypertension. Further empirical research is needed to substantiate these findings and determine the clinical significance of managing wisdom teeth-related inflammation in hypertensive patients.
Stress and Oral Health
Considering the multifactorial nature of stress, its impact on oral health and potential implications for systemic conditions, including hypertension, are gaining increased attention. Research suggests that chronic stress may exacerbate periodontal disease, influencing systemic inflammation and cardiovascular risk factors. Stress-induced neglect of oral hygiene can lead to bacterial proliferation and gingival inflammation. Clinicians emphasize the importance of stress management and maintaining ideal oral hygiene to mitigate these effects. Evidence indicates that individuals with poor stress coping mechanisms exhibit higher levels of oral disease, potentially affecting blood pressure regulation. Expert opinions highlight the necessity of integrating stress management techniques, such as cognitive-behavioral therapy, into dental care protocols. Further investigation is warranted to elucidate the precise mechanisms linking oral health, stress, and hypertension.
The Importance of Regular Dental Check-Ups for Overall Health
Regular dental check-ups play a critical role in maintaining overall health, as they facilitate the early detection and management of oral health issues that can have systemic implications. Dental screenings are essential for evaluating oral hygiene and identifying potential problems such as periodontal disease, which has been associated with cardiovascular conditions, including hypertension. During examinations, dental professionals assess the oral cavity for signs of inflammation, infection, and other anomalies that may contribute to systemic health issues. Evidence indicates that untreated oral infections can exacerbate systemic inflammatory response, potentially impacting vascular health. Additionally, regular check-ups promote the maintenance of ideal oral hygiene practices, aiding in the prevention of disease progression. Extensive dental care, including routine screenings, is indispensable for sustaining both oral and systemic health.
Steps to Take if You Suspect Wisdom Teeth Are Affecting Your Blood Pressure
When individuals suspect that their wisdom teeth may be influencing their blood pressure, it is imperative to employ a systematic approach grounded in clinical evidence. Initially, it is advisable to consult with a dental professional to evaluate the status of the wisdom teeth through radiographic imaging. This assessment will determine if impaction or infection is present, which could potentially contribute to systemic conditions such as elevated blood pressure. Concurrently, monitoring blood pressure levels using a calibrated sphygmomanometer provides objective data to establish any correlation between dental health and hypertension. Should a causal relationship be identified, interdisciplinary management involving both dental and medical practitioners becomes essential. Treatment may include the extraction of problematic wisdom teeth or pharmacological intervention to mitigate hypertensive symptoms.
Frequently Asked Questions
Can Wisdom Teeth Cause Headaches?
Wisdom tooth pain can indeed lead to headaches, often due to referred pain mechanisms. Dental anxiety may exacerbate this symptom, as stress can heighten pain perception. Clinical evidence supports the correlation between dental issues and headache prevalence.
Do Wisdom Teeth Affect Sleep Quality?
Wisdom teeth impaction may contribute to sleep disturbances. Research indicates that oral discomfort can exacerbate sleep apnea symptoms, thereby diminishing sleep quality. Clinical evidence suggests evaluating wisdom teeth as a potential factor in persistent sleep issues.
Are Wisdom Teeth Linked to Ear Pain?
Wisdom teeth can be linked to ear pain due to potential dental infections and nerve damage. When impacted, these teeth may exert pressure on surrounding tissues, leading to referred pain in the ear, highlighting the necessity for clinical evaluation.
Can Removal of Wisdom Teeth Improve Jaw Alignment?
The removal of wisdom teeth can potentially enhance jaw alignment, contributing to improved dental aesthetics. This procedure alleviates crowding and misalignment, as evidenced by clinical studies, promoting a more harmonious occlusion and facial symmetry in patients.
Do Wisdom Teeth Increase the Risk of Gum Disease?
Impacted or partially erupted wisdom teeth can contribute to gum disease due to difficult oral hygiene maintenance. This situation fosters bacterial accumulation, increasing periodontal disease risk, as evidence suggests a link between wisdom teeth and compromised oral health.