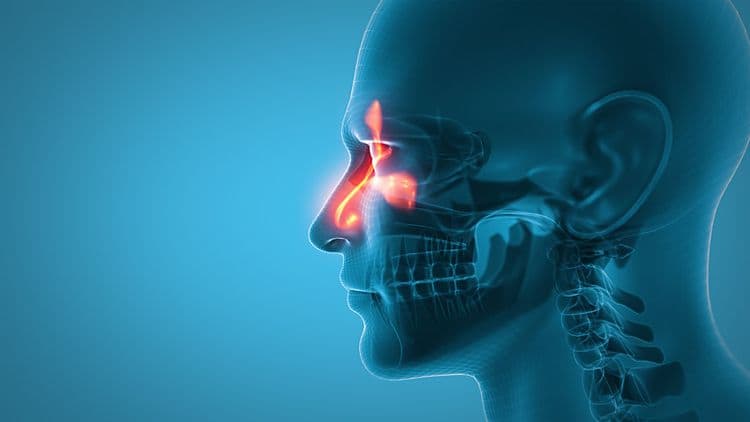
Sinus infections, or sinusitis, can indeed lead to tooth pain, particularly affecting the maxillary teeth due to their proximity to the sinuses. The inflammation and pressure from swollen sinuses can impinge on the maxillary nerve, causing referred pain that mimics dental issues. Understanding the interplay between sinus pressure and oral health is essential for accurate diagnosis and treatment. Recognizing these symptoms may lead to effective management strategies and alleviate discomfort.
Understanding Sinus Infections
Sinus infections, clinically referred to as sinusitis, involve the inflammation of the sinuses, which are air-filled cavities located within the bones surrounding the nose and eyes. Sinusitis presents with sinus symptoms such as nasal congestion, facial pain or pressure, purulent nasal discharge, and reduced olfactory function. These symptoms arise due to obstruction of the sinus ostia and subsequent mucus accumulation. Treatment options for sinusitis are stratified based on etiology and severity. Initial management typically includes saline nasal irrigation and intranasal corticosteroids to reduce inflammation. For bacterial causes, empirical antibiotic therapy is indicated. In refractory cases, adjunctive options include oral corticosteroids or referral for endoscopic sinus surgery. Evidence-based guidelines emphasize accurate diagnosis and tailored therapeutic approaches to optimize patient outcomes.
Anatomy of the Sinuses and Teeth
The anatomical proximity of the maxillary sinuses to the upper teeth roots is a critical factor in understanding the sinus-teeth connection. This spatial relationship can facilitate the transmission of pain signals via shared neural pathways, particularly the trigeminal nerve, leading to referred pain in dental regions during sinus infections. Evidence indicates that inflammation in the maxillary sinuses can exert pressure on the maxillary nerve branches, resulting in perceived tooth pain.
Sinus-Teeth Connection
Nestled within the complex architecture of the human skull, the relationship between the sinuses and teeth reveals a fascinating anatomical interplay. The maxillary sinuses, located above the upper teeth, are particularly significant in this situation. These sinuses are lined with mucosa and play an essential role in sinus drainage and pressure relief. When inflammation occurs, it can lead to congestion and impaired drainage, causing increased pressure within the sinus cavities. The proximity of the maxillary sinuses to the roots of the upper teeth means that such pressure can transmit to the dental structures. This anatomical proximity can result in referred pain, where the discomfort is perceived in the teeth despite originating from sinus-related issues. Understanding this connection is critical in diagnosing sinus-related dental pain.
Pain Transmission Pathways
Although often overlooked, the intricacies of pain transmission pathways between the sinuses and teeth are critical for understanding referred dental pain. The maxillary sinus, situated above the upper teeth, shares close proximity with the roots of the posterior maxillary teeth. This anatomical alignment facilitates potential interactions in pain pathways. Specifically, the trigeminal nerve, responsible for sensory information from the face, has branches—such as the maxillary nerve—that innervate both the sinus mucosa and the dental structures. Nerve connections involving these branches can lead to misinterpretation of pain signals, resulting in referred pain. This phenomenon occurs when sinus inflammation, often due to infection, stimulates these shared neural pathways, causing perceived toothache despite the absence of dental pathology. Understanding these pathways is essential for accurate diagnosis and treatment.
How Sinus Pressure Affects Dental Health
Sinus pressure can greatly impact dental health by exerting force on the roots of maxillary teeth, leading to referred tooth pain. Studies indicate that this pressure is often misinterpreted as odontogenic pain, complicating accurate diagnosis. Understanding the anatomical proximity of the maxillary sinuses to the upper teeth is essential for differentiating between sinus-related discomfort and true dental pathology.
Sinus Pressure Impact
When experiencing sinus pressure, its effects on dental health can be significant and multifaceted. Sinus inflammation, particularly in the maxillary sinuses, can exert pressure on the roots of the upper teeth. This anatomical proximity often leads to discomfort or perceived dental pain, complicating accurate diagnosis. Persistent sinus inflammation may result in increased pressure within the sinus cavities, exacerbating symptoms and potentially affecting oral health. Effective pressure relief is essential to alleviate this impact, often achieved through decongestants or anti-inflammatory medications that reduce sinus cavity swelling. In addition, maintaining sinus health through hydration, humidification, and avoidance of allergens can mitigate the adverse effects on dental structures. Understanding the interplay between sinus conditions and dental health is critical for appropriate treatment and management.
Tooth Pain Connection
The relationship between sinus pressure and dental pain is a significant concern in clinical practice, particularly due to the anatomical overlap between the maxillary sinuses and the roots of the upper teeth. Increased sinus pressure can transmit through the maxillary bone, resulting in referred pain and tooth sensitivity. This phenomenon occurs as the inflamed sinus lining exerts pressure on the nerve endings near dental roots, manifesting as dental discomfort. Clinically, patients may report symptoms mimicking odontogenic pain, yet upon examination, dental pathology is absent. Evidence indicates that sinusitis-induced pressure can exacerbate pre-existing dental conditions, further complicating differential diagnosis. Understanding the interaction between sinus conditions and dental health is vital for healthcare providers to distinguish between sinus-related and true dental pathologies, ensuring accurate treatment.
Symptoms of Sinus-Induced Tooth Pain
Although frequently overlooked, tooth pain can be a symptom associated with sinus infections, specifically when inflammation in the maxillary sinuses exerts pressure on the roots of the upper teeth. This pressure may manifest as tooth sensitivity, primarily affecting the molars and premolars. Individuals often report discomfort during mastication or when exposed to temperature extremes. Sinus symptoms such as nasal congestion, facial tenderness, and postnasal drip commonly accompany this toothache, providing clinical indicators of sinus etiology. Evidence suggests that the maxillary sinus’s anatomical proximity to dental roots can facilitate referred pain, misleading patients into attributing discomfort solely to dental issues. Sinus-induced tooth pain typically fluctuates with head position changes and displays a broader diffusion pattern, distinguishing it from isolated dental pain.
Differentiating Sinus Tooth Pain From Dental Issues
A critical aspect of accurately diagnosing tooth pain involves distinguishing between sinus-induced discomfort and dental issues. Sinus tooth pain is often characterized by diffuse pain impacting multiple upper teeth, directly correlating with sinus pressure fluctuations. This differs from dental issues, where pain typically localizes to a single tooth, often accompanied by heightened tooth sensitivity to temperature or pressure. Evidence suggests that sinus-related pain exacerbates with head movements, such as bending over, due to shifts in sinus pressure, while dental pain remains constant regardless of position. Radiographic imaging can assist in differentiating these conditions by revealing sinus congestion versus dental pathology. Understanding these nuances is essential for clinicians to implement appropriate diagnostic techniques and treatment plans, ensuring the root cause of tooth pain is effectively addressed.

When to Seek Medical Attention
When should individuals with tooth pain consider seeking professional medical attention? Dental professionals and healthcare providers recommend consulting a medical expert when symptoms persist beyond 10 days, as chronicity may indicate a more severe underlying condition. Persistent symptoms such as severe unilateral facial pain, fever, swelling, or nasal discharge unresponsive to over-the-counter interventions warrant immediate evaluation. Additionally, if tooth pain is exacerbated by bending forward or is accompanied by a decreased ability to taste or smell, sinus-related etiologies should be considered. These manifestations often necessitate diagnostic imaging, such as a CT scan, to ascertain the root cause. Prompt consultation guarantees appropriate therapeutic interventions, potentially averting complications such as abscess formation or chronic sinusitis. Early professional assessment mitigates the risk of prolonged discomfort and guarantees ideal care outcomes.
Home Remedies for Relief
In cases where professional consultation confirms a mild sinus infection contributing to tooth pain, individuals may explore non-invasive home remedies to alleviate discomfort. Saline nasal irrigation is a proven natural remedy that can effectively clear nasal passages, reducing sinus pressure. Inhalation of steam, augmented with eucalyptus oil, may offer pain relief by promoting sinus drainage and reducing inflammation. Applying warm compresses to the face can dilate blood vessels, enhancing circulation and alleviating sinus pressure. Hydration plays a pivotal role, as fluids thin mucus, facilitating sinus clearance. Additionally, consumption of anti-inflammatory teas, such as ginger or chamomile, could provide adjunctive benefits. These evidence-based strategies aim to mitigate symptoms, offering a non-pharmacological approach to managing mild sinus-related tooth pain.
Medical Treatments and Interventions
Although home remedies can offer relief for mild sinus-related tooth pain, persistent or severe cases may require medical treatments and interventions. Antibiotic therapy is often employed in cases where bacterial infection is confirmed or highly suspected. This approach aims to eradicate the underlying pathogenic bacteria, thereby alleviating sinus inflammation and associated dental discomfort. Pain management is another critical component, involving the use of nonsteroidal anti-inflammatory drugs (NSAIDs) or acetaminophen to mitigate pain and reduce inflammation. In some instances, corticosteroids may be prescribed to further decrease mucosal swelling. For patients not responding to medical management, referral to an otolaryngologist for potential surgical intervention might be warranted. Clinical evaluation and tailored treatment plans guarantee effective resolution of symptoms.
Preventing Sinus-Related Tooth Pain
Effective management of sinus infections and related tooth pain underscores the importance of prevention strategies to mitigate future occurrences. Preventive measures should focus on reducing known risk factors, such as allergens and environmental pollutants. Implementing lifestyle changes, such as maintaining ideal hydration, can facilitate mucosal clearance and reduce sinus congestion. Regular exercise and a balanced diet enhance immune function, potentially lowering susceptibility to infections. In addition, utilizing humidifiers can maintain appropriate nasal passage moisture, while avoiding tobacco smoke reduces irritation and inflammation. Evidence suggests that nasal irrigation with saline solutions can effectively decrease sinus-related symptoms, thereby reducing the likelihood of associated dental pain. Integrating these evidence-based interventions may greatly diminish the frequency and severity of sinus infections and their dental manifestations.
Frequently Asked Questions
Can Allergies Lead to Sinus Infections and Subsequent Tooth Pain?
Allergy symptoms, including nasal congestion, can obstruct sinus drainage, leading to sinus infections. Sinus infections may exert pressure on upper teeth, causing pain. Effective sinus treatments can alleviate symptoms, reducing the likelihood of subsequent tooth pain.
Are Sinus Infections More Common in Certain Seasons?
Sinus infections exhibit seasonal patterns, often peaking during fall and winter due to increased respiratory illnesses. Maintaining ideal sinus health through preventive measures can mitigate these occurrences, highlighting the importance of understanding environmental triggers and immune system resilience.
Can You Fly With a Sinus Infection Causing Tooth Pain?
When considering flying safety with sinus-related tooth pain, increased sinus pressure changes during flight can exacerbate discomfort. Evidence suggests consulting a healthcare professional to assess risk levels, manage symptoms, and guarantee safe travel under these conditions.
What Foods Might Exacerbate Sinus-Related Tooth Pain?
Spicy foods and dairy products can exacerbate sinus-related tooth pain. Spicy foods may increase nasal congestion, while dairy can thicken mucus secretions, potentially intensifying sinus pressure and discomfort, consequently impacting the perception of dental pain.
Do Children Experience Sinus-Related Tooth Pain Differently Than Adults?
In children, sinus-related tooth pain may present as diffuse discomfort rather than localized ache. Child symptoms can include irritability and difficulty sleeping. Effective pain management involves pediatric-approved analgesics and addressing underlying sinus inflammation with appropriate treatment.